(This is Part 12 of Dr. Pagtakhan’s column, Medisina at Politika, in Pilipino Express)
Former US President Jimmy Carter – a Nobel Peace Prize recipient – and first lady Rosalynn Carter, shown in below photo released on Twitter five days ago by The Carter Center (first reported by Ariella Phillips of CNN), have added their voice and called on the American people to "Please Wear A Mask To Save Lives" as their country continues its struggle against the onslaught of COVID-19. Always filled with a deep sense of humility and humanity, the couple’s call is an appeal, not a mandated order. It makes their posted message with their photo-image wearing masks even more inspiring. And timely for all. The world needs such leadership at this critical time in our common battle against the deadly viral pathogen.

Indeed, wearing a face mask or cloth face covering when out in public as recommended or ordered by public health authorities is one vital yet simple measure to prevent or slow the continuing community transmission of this catastrophic contagion and, thereby, helps reduce the enormous human toll.
Current Human Toll (per John Hopkins University Coronavirus Dashboard, July 13)
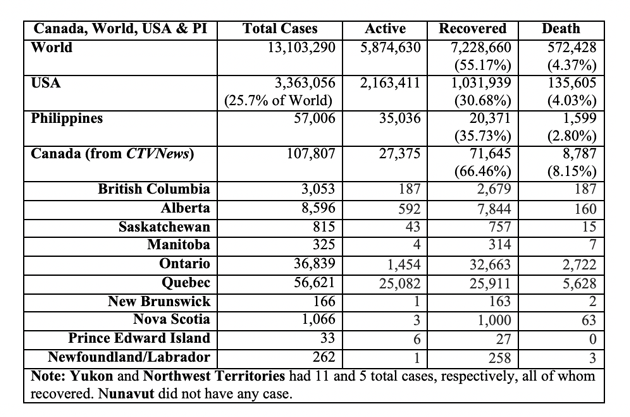
While Canada’s case fatality ratio is double than that of the USA and worldwide, more than two-thirds of the total caseload of patients have now recovered.
Mindful of the community eager for “the great outdoors” and travels, Chief Public Health Officer Dr. Theresa Tam underscored several pointers in a series of recent statements (see PHAC website for details). One key message says “wearing non-medical masks or face coverings is a must when it is not possible to maintain a two-meter distance from others as onboard buses, trains or planes.”
Rationale for Change of Guidance on the Use of Face Mask or Face Cloth Cover
This message is a clear change from what had been conventional wisdom to say “No” to face mask during the early part of the pandemic. Few justifications had been advanced then, including: 1) may give a false sense of protection; 2) may lead to neglect hand hygiene and cough etiquette; 3) mode of transmission was only via close contact with the infected droplets and not airborne; 4) might do more harm if touched with unwashed hands; 5) no definitive study regarding its effectiveness; and 6) the scarce supply had to be reserved for frontline health care workers. The last two justifications ostensibly were difficult to reconcile unless the two environments – the outdoor public and the indoor hospital settings – created a difference in effectiveness for the same medical mask. Note that these justifications were advanced then by the World Health Organization, the Centers for Disease Control and Prevention (USA and Europe), and by the Public Health Agency of Canada.
Meanwhile, use of face mask is nearly universal in Asian countries since Day–1 of the pandemic. Merely a cultural difference?
What the Medical-Scientific Community Now Know
The last three-to-four months into this seven-month pandemic journey have been a great learning experience for both the medical and the research-scientific communities. Not only about development of vaccines and demonstration of useful or non-useful drugs, but also more about this new disease and the behavior of the pathogenic virus – spectrum of clinical severity of illness (mild, moderate, severe, and critical), clinical manifestations (respiratory and non-respiratory signs and symptoms), droplet and aerosolized transmission of virus particles, human-to-human community transmission, shedding of virus and incubation period, carriers of virus with or without symptoms of the disease, availability of rapid diagnostic test, changing age-group vulnerability, and duration of clinical recovery and immunity following infection.
The new body of knowledge that has been gained has informed frontline health care workers and public health authorities to update their approach to management of individual patients and their advisory to the public, respectively. Specifically, the following provide for the rational use of face mask or cloth face covering to help prevent to any degree achievable the further spread of COVID-19:
- The COVID-19 virus easily spreads between infected people even before symptoms appear or without ever developing any;
- The virus can spread through talking or even just breathing in addition to sneeze/cough-induced droplets;
- Heavy breathing and singing can propel aerosolized viral particles farther than two meters (6 feet) and thereby increase the risk of transmission;
- Infectious viral particles could linger in the air for hours and later inhaled;
- Incubation period is long – up to 14 days – and thereby give a wide window of opportunity for people, even before they know they are infected, to infect others; and
- Carriers may be most contagious in the 48 hours before they show symptoms, making transmission even more blind.
Thus, people who look well can have and spread the virus. When they shout, cheer and sing loudly, they produce a lot of droplets and aerosolization and enhance their infectivity. The fact that a person with COVID-19 virus, on average, can spread it to two or three other people makes it twice as contagious as the common flu. Anyone in this type of situation – and that can include anyone of us – is a potential spreader. It is the medical consensus that the main benefit from use of non-medical mask or face cloth covering when out in public is more to protect others. Thus, wearing a mask in public becomes a simple life-saving act of humanity.













